Acne, the complex skin condition it is, comes in many forms. While each pimple is technically formed the same way—dead skin, oil, and debris stick together and block the pores—but from there, it can develop into various types of blemishes. Some are large, red, and tender to the touch (like cysts); others are speckled across your skin, causing textural concerns (blackheads and whiteheads).
Here, we dive into the seven types of acne, the causes, and how to best treat each spot. In terms of remedies, the tips we provide here only scratch the surface, as treating acne requires a holistic view—diet, stress, and sleep can all affect the condition, but this article will focus on specific ingredients for each blemish.

Non-Inflammatory versus Inflammatory Acne
Each type of acne technically falls into one of two categories: non-inflammatory or inflammatory though to be clear, all acne stems from some level of inflammation. A few types are more tender, puffy, and angry than others—those are classified as “inflammatory.” Papules, pustules, nodules, and cysts fall into this category, as they’re all typically red and painful.
“Non-inflammatory” acne, on the other hand, results in subtler mounds—these are your whiteheads, blackheads, and subclinical breakouts. Also known as comedonal acne, the bumps tend to be flesh-toned, aside from blackheads, which are darker in color) It is typically caused by clogged hair follicles and found where the skin is more oily, like the chest, back, and T-zone area of the face.
Non-inflammatory acne can become inflamed later on when there is an overgrowth of bacteria (specifically Cutibacterium acnes1), which can cause the release of inflammatory cytokines and messengers to create clinical inflammation. So again, all acne is inflammation on some level.
Whiteheads

Closed comedones are whiteheads; they look like tiny whitish or flesh-colored bumps on the surface of the skin. Whiteheads are not the large, tender pimples with a big pus-filled center (those are pustules, which we’ll get into later). Rather, because whiteheads are not inflamed, they are much subtler. Think small, fleshy bumps on the skin, caused by dead skin, excess oil, and overall debris blocking the pores.
How to treat it:
• AHAs or BHAs: Sloughing off the dead skin can help you avoid clogging the pores in the first place. Salicylic acid is an ideal option for oily skin (it is oil-soluble allowing it to penetrate into the pores), while AHAs like lactic acid are typically more hydrating and more suitable for those with drier or sensitive skin types.
• Retinol: Retinol and retinoids enhance the skin’s normal turnover process to prevent dead skin cells from accumulating in the pore. Osmosis Skincare offers a range of exceptional Retinal Serums utilizing pharmaceutical grade liposomal retinaldehyde and proprietary nutrients beyond the surface to feed and remodel the skin.
• Get regular peels: There may be a genetic component to nodular acne; that said, if you have a family history, regular, in-office chemical peels can help remove excess dead skin and trigger cell turnover—which, in turn, can help prevent clogged pores and nodules with time.
• Pore-clearing masks: Ingredients like activated charcoal and clay are popular in pore-clearing masks, as these draw out excess oil and gunk from the pores, thus preventing blemishes from forming.
Blackheads

Blackheads form the same way whiteheads do (when the pore becomes blocked with gunk and oil) with one difference: they’re considered open comedones. An open comedone, or blackhead, occurs when the debris is exposed to the air, whereas a closed comedone, or whitehead, occurs when the debris is just under the surface of the skin and not exposed to the air. That oxygen exposure is what makes them turn dark in color.
How to treat it.
Blackheads and whiteheads are cut from the same cloth (aside from the oxidation of the plug), so you can treat them pretty similarly:
• AHAs, BHAs & clays: Cleansers with salicylic acid, clay masks, and chemical exfoliants with alpha- and beta-hydroxy acids can all help to exfoliate the skin and make your skin less prone to developing blackheads. An excellent option here is Osmosis Skincare’s Deep, a detoxifying cleanser that works to remove deep impurities and promotes an invigorating clean.
• Blackhead removers: You can find a slew of market products dedicated to this very issue, from daily toners to blackhead masks to treatment gels (you won’t find any pore strips—as those do not actually unclog the plug at its source).
• DIY masks: Plenty of natural ingredients can gently dissolve dead skin cells and lift debris from the pores, including Cranberry Enzyme, a key ingredient in Osmosis Skincare’s Cranberry Enzyme Mask.
Subclinical acne

While subclinical acne is not a term used in dermatology, it’s used enough in skin care conversations to earn a spot on our list. Essentially, it’s a fancy way of saying “congested skin,” and it’s synonymous with whiteheads.
These flesh-colored bumps never seem to come to a “head,” but they can progress into pimples or pustules if they become inflamed—which can happen if they’re left untreated. They are non-painful and usually do not lead to scarring or skin discoloration.
How to treat it:
• Salicylic acid: BHAs are superb for comedonal acne, as the ingredient can penetrate deep into the pores and help break up the pore-clogging material.
• Retinol: Again, retinol is A+ for preventing comedones as well. Topical retinoids have a comedolytic effect, meaning that they help to prevent and treat clogged pores. This is the result of their ability to increase the turnover of skin cells and reduce the tendency of cells and keratin debris to clump together.
• Benzoyl peroxide: Benzoyl peroxide can kill acne-causing bacteria and help break up pore-clogging agents, like dead skin cells (which can lead to subclinical acne). If you do use retinols, stick to a benzoyl peroxide face wash in the morning, so you can apply retinol at night as when benzoyl peroxide and retinoids (or retinols) are used in combination, they interact causing both to be less effective.
• Get regular peels: There may be a genetic component to nodular acne; that said, if you have a family history, regular, in-office chemical peels can help remove excess dead skin and trigger cell turnover—which, in turn, can help prevent clogged pores and nodules with time.
Papules

Papules are a form of inflammatory acne, they look like solid red bumps, while pustules have pus at the top. These are the stereotypical red-colored bump you may associate with acne—that’s a papule. They start out as a comedone (either closed or open) and become inflamed when bacteria that lives on the skin overgrows inside that clogged pore.
How to treat it:
• Aloe vera: Aloe vera is chock-full of anti-inflammatory vitamins, enzymes, minerals, and amino acids to soothe papules, as well as natural salicylic acids to help unplug the acne at the source. Additionally, aloe has some antimicrobial properties: and aloe used topically in combination with tretinoin cream (a prescription-strength retinoid) was found to be effective in treating inflammatory and noninflammatory acne3.
• Benzoyl peroxide: It kills the acne-causing bacteria, P. acnes, that lives within our hair follicles, and it also helps to break up and remove dead skin cells that clog our pores. This makes the benzoyl peroxide especially helpful for angry papules—it canhelp with comedonal acne but is mainly hailed for shrinking inflammatory pimples.
• Tea tree oil: Tea tree oil has antimicrobial properties and is capable of lowering levels of acne-causing bacteria on the skin when applied to acne lesions. In fact, one double-blind placebo-controlled study found that a 5% tea tree oil gel blend was an effective treatment for mild to moderate acne4. Plus, tea tree oil is anti-inflammatory, which means it has the ability to soothe and relieve irritated, itchy, red, swollen skin. Tea tree oil should always be diluted the potent essential oil with a carrier—you never want to apply it directly to the skin.
• Blue Light Therapy: Blue light therapy that uses light in the 415 nm range is absorbed by porphyrin. The bacteria causing acne, P. acnes contains abundant levels of porphyrin and when the blue light is absorbed an oxygen free-radical is created which is released into the bacteria, killing the bacteria.
Pustules

Again, papules often turn into pustules: When the red papule forms a white, pus-filled head, you now have a tender pustule. People often mistake these white heads as, well, a “whitehead,” but in clinical derm-speak, those are two very different things. It might feel tempting to squeeze the pimple as soon as you see this head forming, but do try to resist this temptation. Self-surgery is not a good idea and it is best to see a professional for extractions—not only can these lead to scarring (which in some cases can be permanent including pitting), permanent dark spots, as well as infections, .
How to treat it:
• Ice: Pustules are pretty swollen, inflamed mounds. And how do we bring swelling down? Ice! Not only does the cool temperature feel produce a soothing feeling, also constricts the circulation, limiting flow to the area and retracting the inflammation. Our professional, in salon acne facials utilize a cold therapy skin stimulation.
• Spot treat: If you have a spot treatment, serum, or mask, that features acne-fighting ingredients (retinol, salicylic acid, tea tree oil, benzoyl peroxide, witch hazel, etc.) such as Osmosis Clarify Retinal Serum, you can always tap it onto the blemish before bed. It’s a great tip to shrink pimples overnight, as the extra dose can help unclog pores and treat the breakout.
• Blue Light Therapy: As mentioned above, blue light in the 415 nm range is absorbed by porphyrin. The bacteria causing acne, P. acnes contains abundant levels of porphyrin and when the blue light is absorbed an oxygen free-radical is created which is released into the bacteria, killing the bacteria.
Nodules

Nodular acne, along with cystic acne are two of the most severe forms of acne, though nodules are firmer than cysts, and more widespread than typical pimples. This type of acne often feels like firm knots under the skin and can be found on the face and body.
In terms of appearance, nodules look like hard lesions that feel like lumps under the skin; and while they may be flesh-toned or red, they’re often pretty painful to the touch.
How to treat it:
• See a holistic esthetician and a dermatologist: First this type of acne is usually the direct result of, or a complicating factor of imbalances in the body including, the gastrointestinal tract (often resulting from food sensitivities / allergies or an overgrowth of harmful bacteria and yeasts – see 7 Foods That Can Cause Acne), hormonal imbalances, etc. Diet is the best place to start with this type of acne. If these initial efforts don’t sufficiently resolve your Nodular acne we recommend you see a dermatologist as OTC acne treatments simply aren’t effective against nodules.
Your dermatologist isn’t likely to provide much assistance as it relates to lifestyle recommendations including dietary factors that could be contributing to your acne. Your dermatologist will be able to prescribe medications, including topicals and systemic therapies such as antibiotics (like tetracycline, mincocycline, or eryhtromycin), oral contraceptives, or isotretinoin (aka Accutane) to treat and prevent any additional lesions from forming.
These medications may help to treat the systems, however, they won’t address the underlying cause of your acne and give you the clear, glowing perfection we all seek (they also all have side effects and other complications)!
• Get regular peels: There may be a genetic component to nodular acne; that said, if you have a family history, regular, in-office chemical peels can help remove excess dead skin and trigger cell turnover—which, in turn, can help prevent clogged pores and nodules with time.
• Look for brightening ingredients: Nodules have a higher risk of scarring. If you notice some scarring or hyperpigmentation, brightening ingredients (think vitamin C or arbutin) can help fade those marks over time. Osmosis Catalyst AC-11 DNA Repair Serum is an exceptional option. This clinically rpoven serum activates the repair mechanisms of our own cells to reverse aging, reduce pigmentation, decrease scar tissue, clear capillaries, and increase skin elasticity.

Cysts
Cystic acne is characterized by inflamed lesions, often large in size, that form deep within the skin—but unlike other forms of acne, they never come to a head on the surface. And unlike hard nodules, cysts can be soft to the touch (in fact, they’re often puffy and tender).
How to treat it:
• Chamomile: This botanical has been an age-old remedy for treating wounds and skin irritations in traditional medicine, and its anti-inflammatory properties may help reduce the painful swelling. When used in topical skin care products, chamomile can help calm and soothe the skin.
Because the inflammation associated with Cystic Acne is so deep, cysts are more prone to scarring. While we’ve repeatedly discussed retinol’s ability to prevent blemishes and breakouts, it can also help decrease acne scarring as well. In addition to exfoliating dead skin cells, retinoid blocks the activity of enzymes behind melanin synthesis, resulting in a more even skin tone. Again we recommend Osmosis Clarify Retinal Serum for the treatment of acne.
• See an esthetician and/or dermatologist: While diet, stress reduction and other at-home methods can help, they shouldn’t be your only plan of action. At the end of the day, cystic acne should always be treated in conjunction with a professional, and the very worst thing you can do for cystic breakouts is to touch, squeeze, or try to pop the lesions.
The Takeaway
Acne is a complex skin condition with several triggers and contributing factors—you can’t expect to treat each spot the same way. Some ingredients are better suited than others for each type of acne, which is why classifying your blemishes is a solid place to start Any treatment plan should include diet, reduction, and other lifestyle factors.
10 Signals Your Body Sends to Tell You Something Is Wrong
Our bodies are incredibly intelligent, often providing us with subtle clues when something isn’t quite right. From minor discomforts to more pronounced symptoms, these signals serve as valuable indicators of our overall health. In this article, we’ll explore ten ways your body may be trying to tell you that something is amiss.
Content is provided for informational purposes only and is not intended as a substitute for medical advice. Seek guidance from your doctor regarding your health and medical conditions.
1. Itching sensations
What else can cause itching all over?
- Skin problems like dry skin, eczema, psoriasis, scabies, burns, scars, insect bites, and hives.
- Internal illnesses like liver or kidney disease, anemia, diabetes, thyroid issues, and some cancers.
- Nerve issues such as multiple sclerosis, pinched nerves, and shingles.
- Mental health conditions like anxiety, OCD, and depression.
- Irritation and allergies from things like wool, chemicals, soaps, or certain medicines.
2. White tongue

White tongue occurs when a white coating develops on part or all of the surface of your tongue. It can be accompanied by symptoms like bad breath, a hairy tongue, and irritation.
Causes can be:
- Neglecting oral care, like not brushing, flossing, or cleaning your tongue often.
- Bad habits.
- Using dentures or injuring your tongue with sharp objects.
- Taking antibiotics, which can cause yeast infections in the mouth.
- Having a diet lacking in fruits and vegetables and high in soft foods.
- Breathing through your mouth.
- Experiencing dry mouth due to medical conditions or certain medications, such as muscle relaxers or cancer treatments.
- Oral thrush, also known as oral candidiasis, is a condition where the fungus Candida albicans builds up on the lining of your mouth. While Candida is typically present in the mouth, it can sometimes overgrow and lead to symptoms.
3. Muscle twitches
Sometimes your muscles act on their own, without you telling them to. They might twitch or contract and have trouble relaxing. Twitches and spasms are most common in areas like your thighs, calves, hands, arms, belly, ribcage, and the arches of your foot. Doctors aren’t always sure why they happen, but a few things can trigger them.
- Your muscles need minerals like potassium and magnesium to work properly.
- Not drinking enough fluids can make your muscles more likely to twitch and spasm.
- Having too much caffeine can also cause muscle twitches in different parts of your body.
- If you have high blood pressure or heart disease, your doctor might prescribe water pills, which make you pee more. This can lower your potassium levels and lead to muscle spasms.
- When nerve cells are damaged, it changes how they talk to each other and to the brain. Twitches and spasms can be warning signs that this common condition is affecting the nerves that control your muscles.
4. Stool as rounded balls
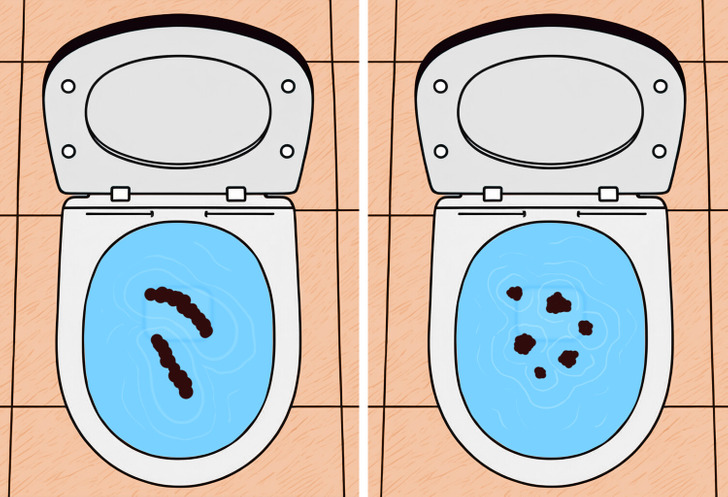
Some things that might make constipation more likely include:
- Feeling worried: Kids and little ones might not go to the bathroom when they’re anxious or if something big changes at home or in their bathroom routine. When parents or caregivers are strict or pushy about toilet training, some kids might hold in their poop.
- Taking certain medicines: Some medicines or pills and stuff like that might make constipation worse. These can be things like antacids, some painkillers, and meds for other conditions like Parkinson’s disease.
- Tummy troubles: If someone has issues like irritable bowel syndrome (IBS) or other stomach problems, they might get constipated. Sometimes, certain foods can also make people feel blocked up.
- Getting hurt: If someone hurts their back or muscles in their belly area, like when having a baby, it might be tough for them to poop. This can slow down how food moves through the body and make poop come out like little pebbles.
- Having a long-term sickness: Some health problems, like diabetes or thyroid issues, can mess with how the nerves and muscles work and make it harder to go to the bathroom.
- How you live: If you don’t move around much or don’t have much activity, you might have a higher chance of getting constipated. Other things like being pregnant, going on a trip, or changing what you eat can also lead to constipation.
- Eating habits: Not eating enough foods with fiber or not drinking enough water can make poop come out like little balls and make it hard to go to the bathroom.
5. White pupil
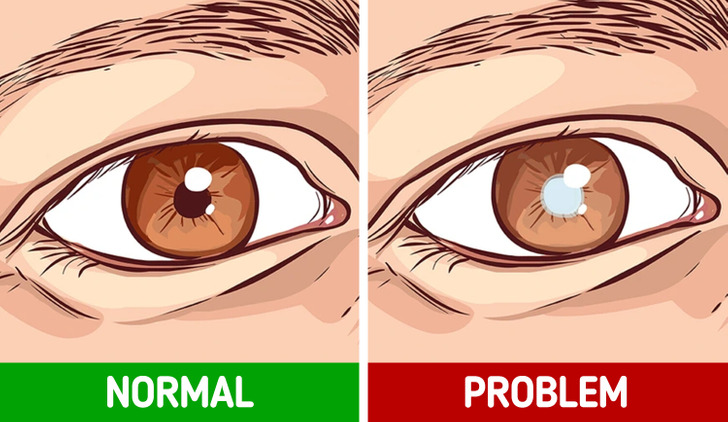
Leukocoria means «white pupil,» and it happens when the pupil of your eye looks white instead of black. It’s more common in kids but can also happen to adults. There are lots of different things that can cause leukocoria, so it’s important to see an eye doctor right away if you notice it. Some things that can cause leukocoria include:
- Cataracts: These are cloudy areas in the lens of your eye that are common as you get older and can be fixed with surgery.
- Retinal detachment: This is when the thin tissue at the back of your eye, called the retina, comes loose. It’s an emergency and needs treatment right away.
- Endophthalmitis: This is an infection inside your eye that needs urgent medical attention. It can lead to blindness if not treated quickly.
- Coats’ Disease: This is when the blood vessels inside your eye become abnormal, causing leaks and buildup of fluid. It can lead to retinal detachment.
- Retinoblastoma: This is a rare type of eye cancer, mostly seen in kids. Leukocoria is one of its main symptoms, along with poor vision and other eye problems.
- Power difference: Sometimes, one eye might look different because it has a different power than the other one. This isn’t usually serious and can be fixed easily.
6. Pale nails
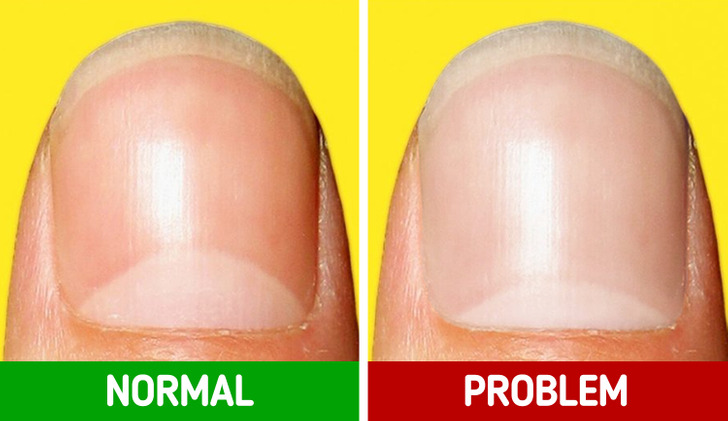
Are your nails pale or white? This might indicate a low red blood cell count. White nails can also suggest various conditions such as trauma, liver disease, diabetes, an overactive thyroid, heart failure, heavy metal poisoning, chemotherapy, or a lack of nutrients in your diet.
If your nails are mostly white with a thin pink strip at the tip, you might have Terry’s nails. This condition can occur as a result of aging, but it could also be a sign of underlying health issues such as diabetes, kidney, liver, or heart disease.
7. White finger

Raynaud’s disease makes parts of your body, like fingers and toes, feel numb and cold when it’s chilly or when you’re stressed. It happens because the small arteries that carry blood to your skin get narrow, reducing blood flow to those areas. This narrowing is called vasospasm.
Raynaud’s disease is more common in women than men and tends to affect people who live in colder places.
8. Floaters and flashes of light in eyes

See if you have floaters and flashes in your vision. Floaters can appear as small dark dots, squiggly lines, rings, or cobwebs. Flashes are like sudden bursts of light.
Floaters and flashes are common, especially among older people. They usually happen because of a harmless process called posterior vitreous detachment (PVD), where the gel inside your eyes changes. Sometimes, they can also be caused by retinal detachment, which is serious and needs treatment to prevent permanent vision loss. Floaters and flashes can also occur for no clear reason.
9. Puffy face

Sometimes, your face might swell up because of health issues like injury, infection, or allergies. Some of these reasons can be really serious.
You might wake up sometimes with a puffy face. This could happen if something pushes on your face while you sleep. But if your face gets swollen or puffy because of an injury or if it happens often, it could be a sign of a health problem.
Facial swelling isn’t just about your face; it can also affect your neck or throat. If your face swells up and there’s no injury, it could be a sign of a serious health problem. It’s best to have a doctor check it out.
10. Vivid dreams

So, why do we have intense dreams? Scientists aren’t totally sure, but they think a few things might be involved.
- When life gets tough, whether it’s problems with friends, family, school, or work, it can make us feel stressed or anxious. Big life events like getting married or buying a house can also lead to vivid dreams. Traumatic experiences, like losing someone close to us or being in a bad accident, can also cause intense dreams. Anxiety, especially, is linked to having scary and intense nightmares.
- Not getting enough sleep because of issues like insomnia or narcolepsy can make vivid dreams more likely. Changes to our sleep routine, like traveling to different time zones or not getting as much sleep as usual, can also increase the chances of having intense dreams.
- Some medicines, like certain antidepressants, blood pressure pills, and drugs for Parkinson’s disease or quitting smoking, have been linked to vivid dreams.
- Bad habits can lead to vivid dreams, often bad ones.
- Mental health problems like depression or schizophrenia, as well as physical illnesses like heart disease or cancer, can also cause intense dreams.
- Being pregnant can mess with our hormones, sleep, and emotions. Lots of pregnant women say they have really vivid dreams, especially in the early months of pregnancy.
Maintaining good health is essential for a happy, balanced life. When we’re physically and mentally well, we have the energy to pursue our goals, enjoy relationships, and engage fully in life. Prioritizing exercise, healthy eating, adequate sleep, and self-care practices lays the foundation for overall well-being and fulfillment.